This is the fourth blog in a series by Maggi Bradley QN.
About me
 Based in the North West of England at the point where the Irish Sea becomes the River Mersey, I am a wife, a mother, a proud owner of two Puggles and, for more than 35 years I have been a midwife, then a General Practice Nurse. Additionally, I work with my regional training hub where I am responsible for encouraging student nurses to enter General Practice, then supporting them in their continuing development. I am also proud to call myself a Queen’s Nurse.
Based in the North West of England at the point where the Irish Sea becomes the River Mersey, I am a wife, a mother, a proud owner of two Puggles and, for more than 35 years I have been a midwife, then a General Practice Nurse. Additionally, I work with my regional training hub where I am responsible for encouraging student nurses to enter General Practice, then supporting them in their continuing development. I am also proud to call myself a Queen’s Nurse.
Are you sitting comfortably…?
So, with the tech in place, the training done, the rehearsals completed, and the team ready to go, it was time for our first Video Group Consultation (VGC). The management of patients with asthma is my area of expertise, and my comfort zone, so I decided to start here. Invitations went out to asthma patients who we thought would be most comfortable using the technology and who usually find it difficult to attend the surgery during the working day.
With great anticipation and jangling nerves, the faces of patients began to appear on our screens. We’d invited six people, but only two joined. This wasn’t expected but we pressed on, and it worked successfully, with real patients! We even found that it was great fun on both sides of the screen, with one patient remarking, “When we move away from lockdown I would be happy to continue with this process if it means not having to leave work or schedule time away.”
It worked, and we were determined to continue.
Peer learning
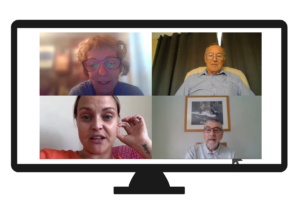 Two more VGCs were arranged and this time we removed our filters. Instead of assuming which patients would be best equipped and willing to use a technology-based solution, we invited anyone who was eligible. And they joined. And when we saw each other for the first time since lockdown, the patients were very excited, and so was I.
Two more VGCs were arranged and this time we removed our filters. Instead of assuming which patients would be best equipped and willing to use a technology-based solution, we invited anyone who was eligible. And they joined. And when we saw each other for the first time since lockdown, the patients were very excited, and so was I.
These consultations were easy to manage and a pleasure to experience. Technology wasn’t a barrier, in fact, participants had grown used to using screens to communicate with family members during lockdown so this was a natural extension. Even I was getting used to online etiquette, though it was daunting to demonstrate correct inhaler technique to a screen of so many concentrating faces!
It was also notable that with more people involved, group dynamics had kicked in and peer learning had organically begun. They weren’t just benefiting from my healthcare advice; they were sharing real-life personal experiences in a safe and enjoyable environment, and I was learning to.
We sought feedback on a regular basis and used this learning to adjust and improve the experience. This included altering the invitation letter, adjusting the meeting duration, and adding a few minutes at the end of every session to reflect on what went well, and what could be further improved.
Expanding the service – cancer patients
Now, more comfortable in the process, we expanded our range and began hosting VGCs for patients with cancer. These proved to be some of the most memorable sessions I experienced. Lockdown had caused some cancer treatments to stop and face-to-face discussions with Health Care Professionals had ceased. Even the most difficult diagnoses were delivered by phone. Patients were understandably anxious and felt alone.
In normal times, Primary Care will conduct a Cancer Care Review within twelve months of diagnosis. With face-to-face visits no longer viable, the VGC model looked like it might help to bridge the gap, but I was worried the different dynamics of such a group would limit success. For some this would be the first time they would talk about having cancer; would they want to speak? Would they want to share time with others in the same situation? How would a group react if a member became distressed or angry? I took a breath and decided to give it a go.
What we experienced, pretty much straight away, was remarkable. Patients who had been living with cancer for a long time were sharing experiences with those who were newly diagnosed. Tips were given on matters that had never even occurred to me, and were well received. We went on to include advice from Macmillan Cancer Care and other specialist support services, covering matters such as self-management, diet, exercise, treatment, and financial/benefit support.
These people weren’t wallowing in their diagnosis, they were seeing the light of a future which they badly needed. They weren’t morbid or difficult, they were laughing, listening and no longer alone. We have now rolled out VGCs for patients with cancer across the entire Primary Care Network and surgeries regularly refer their patients to our VGCs.
New mothers
VGCs for Postnatal women also proved to be a success. Now, it is quite common for a new mum to attend a postnatal review from the comfort of an armchair, in their own house, whilst feeding the baby. Once again, the group element plays an important part in the success of these meetings, as more experienced mums openly share advice and tips with those who are less experienced in parenting. We discuss parent health, coping strategies, mental health, and I can identify areas where one-to-one nursing care would be beneficial. Recently one mother who was five minutes late to a meeting explained that an emergency bath had been required for her twins following explosive nappy issues! She wouldn’t have made the meeting if she had had to get the bus to the surgery.
Changing life for the better
Another anecdote came from a diabetic patient, an active 70-year-old farmer. He was extremely anxious about using technology but wanted to attend a VGC for people with type one and two diabetes. Determined to overcome his inexperience in using computers, he asked his daughter-in-law to help and soon enough he joined us and became an active member. In fact, after listening to a group conversation about diabetic hypos and how a glucose monitoring system had been life-changing for younger group members, he recognised that this may help him and asked for my support to make this happen. Within a couple of months this was in place, his blood sugars were in control, and he openly says that the advice he received during the meeting changed his life for the better.
We’re now at a point where VGCs are part of normal life, a critical additional tool to the Primary Care toolkit. But it’s not been easy. There have been technological, personal, cultural, and environmental issues/pressures to overcome. I now realise this is normal and to be expected when change is necessary. I’ve also learned that these are barriers, not stop signs, and can be overcome with agile working, determination, adaptable processes, and good people.
My VGC journey was only possible because I worked with a fantastic group of student nurses who were willing to lead change in difficult times. My sincere hope is that these students have learned with me about the value of innovation, the importance of sustainability, the critical importance of good communication and the determination to succeed.
As my Topol Fellowship draws to an end, my final blog will explain how the Topol experience has forever changed me as a Nurse and a person.
Maggi Bradley
General Practice Nurse, Queen’s Nurse, HEE Topol Digital Fellow 2021
Follow Maggi on Twitter: @nursemaggi
Other blogs in the series by Maggi:
- I’m Far Too Old for this Covid-19 Business!
- My Topol journey
- And on to my project…
- The End of the Beginning
